With patient adherence thought to be lower than 50% 1, drug companies are increasingly maximizing dosages to bridge the gap at population scale – but are we overdosing individual patients as a result?
The industry’s tendency to always aim for the highest possible dose in the therapeutic window to compensate for missed doses runs the risk of increasing side effects at the same time.
In this article, Bernard Vrijens, CEO & Scientific Lead at AARDEX Group explores the challenges facing the industry in dose selection and properly understanding drug forgiveness as a means of canceling out poor patient adherence.
Forgiveness of the drug in question can hugely influence the effects of medication taken sporadically – useful when estimates gauge overall patient adherence with prescribed medications at less than half, but there is a need to scrutinize dose selection before we overdose as a nation.
A Closer Look at Patient Adherence
Adherence to medication is dependent on three factors: initiation, implementation, and persistence. Consequently, non-adherence can take several forms: the patient does not initiate treatment; they delay, omit, or take extra doses during the implementation of the dosing regimen; or they discontinue treatment.
Results are therefore clearly linked to the relevant scenario: where patients don’t initiate a medication plan or discontinue, the drugs don’t work or stop working. But for patients who implement a sporadic dosing regimen, the drug’s forgiveness has a vital role to play.
Understanding the Concept of Drug Forgiveness
Adherence is just the first stage in generating the drug response, which is also dependent on pharmacokinetics (relating to drug absorption, distribution, metabolism, and excretion) and pharmacodynamics (referring to the biochemical and physiological effects of drugs and their mechanisms of action).
To understand medical adherence, let us consider an example where, over a two-year prescribed dosing regimen, doses were missed on 115 days in total (18%) – but doubled up on 14 occasions (2%), meaning 84% of the prescribed doses were taken.
Connected packages can capture every dose taken, allowing for the pharmacokinetics, or drug exposure, to be fully monitored depending on the adherence profile.
The discrepancy between the ideal dosing regimen and the actual dosing regimen can mean sub-optimal dosing, increasing the variability of concentrations in the exposure process.
Explored within the framework of pharmacodynamics, lower drug concentrations mean lower efficacy; as the drug concentration increases, the efficacy increases, and typically there is a plateau. Safety issues follow a similar curve: at higher concentrations, safety concerns arise and then plateau (see Fig 1.)
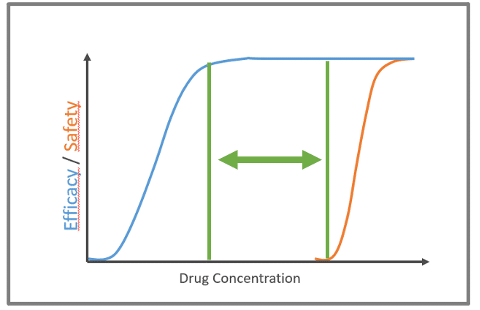
The Challenge Facing the Industry
Identifying the correct dose, and the dosing regimen, that will bring patients within the correct therapeutic window is a monumental challenge facing the pharmaceutical industry today.
Varying adherence creates drug-specific issues of efficacy, safety, and drug resistance. It is imperative that, even if there is some variability in concentration, maximum effects can still be gained without compromising on safety.
What is Allowed Deviation?
Forgiveness (F), or the allowed deviation, in medication adherence, is defined, in symbolic terms2,
as the difference between the medication’s post dose duration of beneficial action (D) and the prescribed dosing interval (I): F = D – I. The larger is F, the most forgiving is the medication.
Why does Drug Forgiveness Matter?
With an unforgiving drug, as soon as a patient deviates from the dosing regimen it will lose efficacy rapidly. A more forgiving drug still offers a response when adherence slips.
The result is a rising tendency in the industry to always aim for the highest possible dose in the therapeutic window to compensate for potentially missed doses. This runs the risk of exposing people to side unnecessarily high levels of the drug, which can lead to exposure-related short- and long-term side effects and adverse events. It’s important to note here that such toxicity and safety issues are among the main reasons for non-persistence, which is an important form of non-adherence.
A study published in The Lancet in February 2022 found that because of longer half-lives and higher genetic barriers to resistance, modern antiretroviral therapy medications are more forgiving of missed doses than ever before. This improvement has two potential benefits: first, more people with HIV could achieve virological control with moderate adherence; and second, some people with HIV with full adherence could safely reduce the number of antiretroviral therapy doses while maintaining virological control. For some, this resulted in a four-days-on and three-days-off maintenance treatment strategy3, highlighting the level of forgiveness the drugs provide.
Controlling Intake in Prisons
In prisons, where compliance with prescribed medications among inmates is often 90% or higher, physicians have reported that dosages can be lowered when intake is controlled otherwise it can lead to toxic patients4. Writing in MedPage Today in 2018, Jeffrey E Keller MD detailed how the fact that inmates are much more compliant with taking their medications when in jail than when they are at home “often results in important medical consequences – patients can get hurt”.
Their new regular dosing regimen can result in what he has labeled ‘the Compliance Trap’ when previously erratic adherence shifts to a regular regime and, as a result, drug levels can become toxically high. So, according to Dr Keller, “the only way to know for sure is to check appropriate monitoring levels a week, say, after they arrive in the jail”.
He notes that this had been due to physicians continuing to prescribe higher doses to meet the optimal levels without understanding the patient’s level of non-adherence. But it reflects the wider trend in the pharma industry that dosing is not always optimal – it is simply maximal.
What is the solution?
Understanding drug forgiveness offers a new scenario: how optimal medication adherence can mean optimal drug response.
With an unforgiving drug, sub-optimal medication adherence will result in a sub-optimal drug response. But with a forgiving drug, even sub-optimal medication adherence will still see the desired outcome: optimal drug response. You prescribe and it works.
Moving Towards Optimized Forgiveness
Misunderstanding forgiveness, or over-mitigating for its effects, runs the risk of overdosing the entire population leading to increased side effects for some to achieving the right average level of efficacy for the majority.
We need forgiveness in treatment because not every patient will behave like a robot and stick rigidly to their daily regime – but we don’t need too much forgiveness, as over-exposure can, conversely, result in adherence-sapping side effects and toxicity. What we need is an optimized forgiveness that balances the drug’s efficacy with real-life medicine-taking behavior. To date, pharma has not had the best track record in this regard – as demonstrated by the significant number of post-marketing dose reductions that take place once extended data collection offers a more representative picture of real-world adherence patterns and drug efficacy.
For continuity of drug response, the only way to have optimized forgiveness and effective therapies is to balance pharmacometrics considerations – like disease, drug formulation, dose quantity, the interval between doses, and position in the therapeutic window – with behavioral considerations, like the most frequent deviations in medication adherence or how to best support patients to effectively manage adherence. Instead of running the risk of overdosing patients, a better route is to collate data on behavioral considerations like acceptable deviation or offer instructions on how to cope with non-adherence to boost compliance and mitigate the need for forgiveness.
ENDS
References:
- https://pubmed.ncbi.nlm.nih.gov/22964778/
- Clinical Pharmacology & Therapeutics: Vol 88 Number 4. L.G. Osterberg et al Oct 2010
- https://www.thelancet.com/journals/lanhiv/article/PIIS2352-3018(21)00300-3/fulltext
- https://www.medpagetoday.com/opinion/doing-time/73738
About the Author
Bernard holds a PhD from the Department of Applied Mathematics and Informatics from Ghent University, Belgium. As Scientific Lead at AARDEX ® Group, Bernard oversees the research and development of sophisticated analytical methods for monitoring participant medication-taking behaviours. Along with providing guidance on adherence to Pharmaceutical, BioPharma, and Academic organizations, Bernard is a founding member of the International Society for Patient Adherence (ESPACOMP) and is an active member of several EU and US-funded consortiums that focus on adherence. Having co-authored several book chapters, over 100 peer-reviewed scientific papers, Bernard is considered an expert in his field.



